Welcome to a journey of discovery. As an experienced healthcare professional, I have come across numerous cases of people dealing with vein pain. If you’re wondering, “Why does my veins hurt?“, you’ve come to the right place. Through this article, you will gain insights into the possible causes of your discomfort and the steps you can take towards relief.
So, why are your veins hurting? The pain in your veins can be due to a myriad of issues such as Chronic Venous Insufficiency, Varicose and Spider Veins, or Peripheral Artery Disease (PAD). These conditions affect the flow of blood in your veins, leading to discomfort and pain. By addressing these underlying conditions, you can alleviate the pain and restore normalcy to your life. So let’s dive deeper into understanding these causes and their respective remedies. Don’t stop reading now, the solution to your pain is just a few scrolls away!
What Causes Vein Pain?
Vein pain, a common complaint among many people, can be attributed to various health conditions. The discomfort arises when there is an issue with the circulation of blood in your veins. This could range from minor issues like a mild strain or injury to more serious conditions such as blood clots or varicose veins. Understanding the root cause of your vein pain is the first step towards finding an effective solution.
In some cases, vein pain could be a symptom of Chronic Venous Insufficiency (CVI). This condition occurs when the valves in your veins, which prevent blood from flowing backward, fail to function properly. As a result, blood accumulates in the veins, causing them to enlarge and become painful. Peripheral Artery Disease (PAD) is another condition that can cause vein pain. In PAD, the arteries narrow, reducing blood flow to your limbs and causing pain, especially during physical activities.
According to a study published in the Journal of Vascular Surgery, nearly 40% of adults in the United States suffer from Chronic Venous Insufficiency. Furthermore, the American Heart Association reports that approximately 8.5 million people in the U.S. have Peripheral Artery Disease. These statistics underline the prevalence of these conditions, highlighting the importance of understanding their symptoms and seeking timely medical attention.
The Link Between Chronic Venous Insufficiency and Vein Pain
Chronic Venous Insufficiency (CVI) is a condition that affects the functionality of your veins, particularly those in the lower limbs. In CVI, the veins fail to efficiently circulate blood back to the heart, leading to the accumulation of blood in the vessels. This condition is one of the primary causes of vein pain, and understanding its dynamics is crucial in managing and treating the discomfort associated with it.
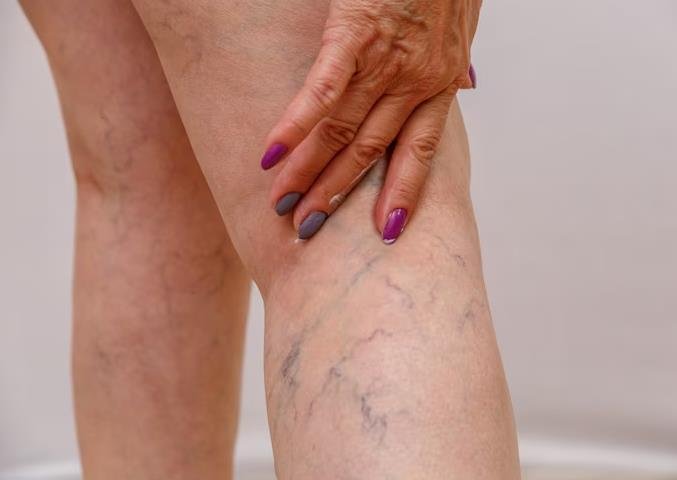
Why Does My Veins Hurt: A Comprehensive Analysis
In a healthy vein, one-way valves ensure the unidirectional flow of blood towards the heart. However, in CVI, these valves malfunction or become damaged, causing blood to pool in the veins. This pooling can lead to an increase in venous pressure, venous enlargement, and subsequently, the manifestation of pain. The pain experienced due to CVI is typically a dull ache or heaviness in the legs, often worsened by prolonged standing.
Apart from pain, CVI can also lead to other symptoms such as swelling, changes in skin color, and the development of varicose veins. It is reported that approximately 6% of men and 9.4% of women worldwide suffer from CVI, emphasizing the significance of understanding this condition in relation to vein pain.
How Varicose and Spider Veins Contribute to the Pain
Varicose and spider veins are common vascular conditions often associated with vein pain. These conditions occur when the veins become enlarged or twisted, disrupting normal blood flow. The discomfort you experience is largely due to the increased pressure exerted on the walls of these affected veins.
Varicose veins are larger, often visible under the skin, and may appear as bulging, bluish cords. They typically occur in the legs and can cause symptoms like aching, heaviness, and pain. On the other hand, spider veins are smaller, closer to the skin surface, and can appear anywhere on the body. While they usually cause less discomfort than varicose veins, they can still contribute to a feeling of generalized vein pain.
According to the U.S. Department of Health and Human Services, about 55% of women and 45% of men in the United States suffer from some form of vein problem. Varicose veins affect around 50% of people aged 50 years and older, and spider veins occur in up to 15% of both men and women. These statistics illustrate the widespread nature of these conditions and their potential contribution to vein pain. It’s important to understand the role they play in vascular health and to seek appropriate treatment if you’re experiencing discomfort.
Peripheral Artery Disease (PAD) and Its Impact on Vein Health
Peripheral Artery Disease (PAD) is a circulatory condition where narrowed arteries reduce blood flow to your limbs. When you develop PAD, your extremities — usually your legs — don’t receive enough blood flow to keep up with demand. This causes symptoms, most notably leg pain when walking, which is known as claudication.
PAD can also contribute to changes in the skin color on your feet, poor nail growth, decreased hair growth on toes and legs, and slow healing of wounds. Over time, PAD can affect the health of your veins by putting additional pressure on them due to inadequate blood flow. This can lead to conditions like varicose veins and deep vein thrombosis, which can cause significant discomfort and pain.
The American Heart Association estimates that PAD affects around 8.5 million Americans. It’s a major risk factor for heart attack and stroke, and it’s critical to be aware of its impact on overall vascular health. Regular check-ups and lifestyle modifications can help manage the effects of PAD and improve your vein health.
Understanding Vascular Pain and Its Symptoms
Vascular pain is a term used to describe discomfort that arises from issues related to the circulatory system, which includes the veins and arteries. This type of pain can be attributed to a variety of conditions ranging from Peripheral Artery Disease (PAD) to varicose veins. The nature of vascular pain can vary widely, depending on the underlying condition causing it.
Common symptoms of vascular pain include aching or throbbing in the affected area, numbness or weakness, and changes in skin temperature or color. In more severe cases, such as in deep vein thrombosis, symptoms can include swelling and redness. It’s also crucial to note that symptoms can manifest differently depending on the specific vascular condition at play.
According to the Centers for Disease Control and Prevention (CDC), PAD, a common cause of vascular pain, affects about 8.5 million people in the United States. With such a significant number of people experiencing vascular pain, understanding its symptoms is essential for early diagnosis and effective treatment.
Practical Remedies for Painful Hand Veins
Painful hand veins can be an uncomfortable and often alarming experience. This discomfort can result from various factors, including aging, injury, or underlying health conditions such as varicose veins. While serious cases may require medical intervention, there are practical remedies you can employ at home to alleviate the pain associated with this condition.
Here are some steps you can take to manage painful hand veins:
- Stay Hydrated: Drinking plenty of fluids helps maintain your blood’s viscosity, promoting better circulation.
- Exercise Regularly: Regular physical activity encourages better blood flow, which can alleviate vein pain.
- Elevate Your Hands: Whenever possible, elevate your hands to reduce swelling and discomfort.
- Apply Warm Compresses: Warmth can help soothe painful veins and promote blood flow.
- Wear Compression Gloves: These specially designed gloves apply pressure to your hands, promoting better blood circulation.
While these remedies can help manage the symptoms of painful hand veins, it’s important to consult a healthcare professional if your symptoms persist or worsen. They can provide a proper diagnosis and recommend suitable treatments based on your specific condition.
Conclusion
Understanding the dynamics of vein pain and its related conditions is crucial in managing and treating the discomfort effectively. From chronic venous insufficiency to peripheral artery disease, these conditions can significantly impact your quality of life. However, with the right knowledge and resources, you can take proactive measures to maintain your vein health and lead a comfortable life.
Remember, while home remedies can provide temporary relief, it’s always important to consult with healthcare professionals for proper diagnosis and treatment. With the right care and attention, you can manage these conditions successfully and keep the smile on your face.
Frequently Asked Questions
[faq-schema id=”1252″]
















